Although we treat all forms of cardiac arrhythmia, atrial fibrillation is the commonest and most confusing for patients so here is some more information:
Overview of Atrial Fibrillation (AF)
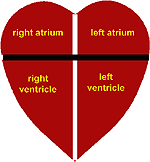
The anatomy of the heart
The heart is a pump which is divided into two sections, the atria and ventricles, and into two halves the left and right. This means that the heart is divided into 4 chambers. The atria pump blood into the ventricles and thus have a relatively small job to do, and the ventricles pump blood around the body and thus take on most of the work. The atria are therefore thinner and smaller than the muscular ventricles. The right heart pumps blood through the lungs to get oxygen into it and the left heart pumps blood around the body including the brain.
The electrical system of the heart
Normally the atria pump blood into the ventricles before the ventricles pump blood around the body, therefore the atria and ventricles are working in sequence. The heart normally beats 60-80 times a minute however this gets faster if you need your blood to move through your body more quickly, for example during exercise. To allow the chambers to pump in sequence and for the heart to go faster and slower it has an electrical timing system.
It is this system that is faulty when people have abnormal heart rhythms, also known as ‘arrhythmias’. A small bunch of cells situated at the top of the heart, the sinus node, sends an electrical impulse out at about 60 to 80 times a minute (hence your heart rate is 60 to 80). This electrical impulse then washes like a wave across the atria from right to left being conducted from cell to cell and making the cells contract causing the atria to squeeze. The atria and the ventricles are insulated from one another (black line) so when the electrical wave hits this insulation it dies out and the cells await the next impulse from the sinus node.
The atria is electrically connected to the ventricle by the atrioventricular node and bundle branches which are electrical “motorways” that spread the electrical wave very quickly through the ventricles causing them to contract. The wave therefore washes through the heart from top to bottom before dying out, until the next impulse from the sinus node.
The AV node has a rate limiting function. It will allow your heart to get up to 200-220 bpm if the circumstances require it. However it won’t allow your heart rate to exceed that and therefore protects or firewalls the ventricle from the atrium ensuring that the ventricles will continue to pump regardless of AF which is limited to the atrium.
The AV node may still send more signals into the ventricle during AF than is appropriate if one is not exercising, and it will also send them irregularly (because the AF waves hitting the AV node are irregular). This explains why one pulse is irregular and may be faster than is expected. This is not the AF but the ventricle producing a pulse and heart beat in response to the AF.
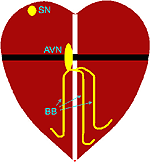
Key: SN sinus node, AVN atrioventricular node, BB bundle branches
Atrial fibrillation (AF)
In AF the sinus node has lost control of the heart. Rather than a single electrical wave emerging from the sinus node, there are many groups of rogue cells which are generating their own electrical waves. Hence there are lots of smaller waves which are continuously and chaotically wandering around the atrium. These rogue cells are usually found in the left atrium, most often at the junction of the pulmonary veins (the veins which bring blood back to the heart from the lungs).
To see a recording of atrial fibrillation in a human click here. This is a recording made over a period of a 10th of a second with a mapping system called non-contact mapping and is of a human left atrium. The video shows 2 views of the left atrium (front and back) with electrical waves as white and coloured areas passing over the surface of the atrium (coloured purple when not being activated). In this recording, which is slowed down to help the viewer see a bit of what is going on, one can see how complex atrial fibrillation is.
In the presence of these chaotic electrical wavefronts, the atria do not contract but appear to shiver or fibrillate. There is very little muscle in the atria and there are no valves to stop blood going back the way that it has come, if the atria do contract. This therefore may explain when the atria stop pumping during AF, nearly half of people are unaware that this has happened.
The lack of atrial contraction may however in some people reduce the pumping efficiency of the heart. The atria can be likened to a turbo-charger on a car. If your car is sitting at the traffic lights it does not use the turbo. The effect of the atrial contraction is similarly minimal when someone is resting, because all the blood flows into the ventricle on its own without the atrium. However when the traffic lights go green and the driver puts their foot on the pedal they will notice immediately that the turbo is not working because the car will be much slower than normal. The same may be true for the heart, particularly in active people.
Many patients notice that they are in AF because they cannot do as much as they could when they were in normal rhythm. Because AF is a chronic condition, patients get used to this lack of function and forget what it was like when they were in normal rhythm. It is not uncommon for patients to be surprised at what they can do when restored to normal rhythm and feel worse if they return to AF because they have been reminded what it is like to be in normal rhythm.
As explained before, the atria are connected to the ventricle via the electrical connection the AV node (see figure). The AV node will respond to the chaotic electrical signals in the atrium and try to keep up. The ventricle (and therefore the heart beat and pulse) will contract irregularly, rapidly and with a varying intensity, because for each contraction of the ventricle will pump out a different volume of blood.


