What is Catheter Ablation for Atrial Fibrillation?
Catheter ablation is a minimally invasive procedure designed to target the regions of the atria that allow the AF to initiate or sustain itself. It is more targeted than drug therapy which is why in every research trial published to date, it has been superior in efficacy to drugs in eliminating AF. This means that while there is no guarantee of success, there is a good chance that suitable patients will do well after an ablation and have their vulnerability to AF very significantly reduced.
Pre-Operative Advice
Important measures that you can take to improve the chances of an AF ablation being successful are:
- Reduce or eliminate alcohol
- For some patients this can be an important promoter of AF)
- Lose weight and improve fitness
- • Studies have shown that AF burden will reduce if overweight patients are able to lose weight. They may also suffer less sleep apnoea (obstruction of the air passages during sleeping leading to snoring and poor quality sleep) which is also a promoter of AF.
- Ensure their blood pressure is well controlled (target an average of 140/90 or less).
- The British Society of Hypertension gives good advice on this.
Pre-Operative Consent & Tests
Prior to your procedure we will talk to you about the ablation the likely outcomes and risks for you. We will send you a consent form to read and sign. Depending on whether you are decided yet and are having the procedure scheduled soon we may also arrange for you to have some blood tests. We will also ensure that you are on an anticoagulant drug. We may give some patients an anti-rhythm drug to reduce the chance of them getting AF during the inflammation that occurs in the first 6 weeks after the ablation.
Before the Procedure
Before the procedure you will be asked to starved for at least at least 3-6 hours so that your stomach is empty and can be safely sedated. We perform a transoesophageal echo at the start of the procedure, partly to guide the procedure, increase its safety and reduce the amount of x-rays we use. It is also used to make sure there are no clots in the heart before we start. If it does show that there is a clot in the heart (very unusual) then we delay the procedure for a few weeks to allow the anticoagulants to dissolve the clot.
The procedure is usually done as a day case, but sometimes as an overnight stay in hospital. The local anaesthetic is introduced into the top of the leg where we pass that catheters and this reduces the discomfort here after you wake up from the procedure.
Atrial Flutter Sufferers
Some people also suffer from atrial flutter as well as AF and for them we may also perform an ablation of the isthmus between the tricuspid annulus and inferior vena cava which will also prevent atrial flutter occurring after the procedure..
Medications
anticoagulants, but because it has a different method of action, it does not have the stroke prevention effect (it is good at preventing heart attack but not AF related stroke). Therefore, if people take aspirin for stroke prevention in AF they are taking all the bleeding risks but getting none of the benefits of protection. The good news is that there are now a range of anticoagulants available that work very well to prevent stroke in AF. Not all people with AF require anticoagulation any or all of the time, we will be able to advise you individually. All patients undergoing ablation are given anticoagulants to prevent clots forming during the healing process.
The anticoagulants commonly used at the moment include warfarin, dabigatran, apixaban, and rivaroxaban. The latter three are collectively termed DOACs (direct oral anticoagulants) and used to be called NOACs (novel oral anticoagulants – this term is now falling out of used because they are not novel any more).
Warfarin is the drug with the longest history, but does require regular blood tests to ensure you are receiving the best dose for you. This is because its action varies from patient to patient and over time because many things can influence its behavior like changes in diet. Patients often have arrangements at a clinic or hospital close to where they live or work for this, but if you do need help with the monitoring and management of your medication we have a team of teaching hospital consultants who can look after you.
The DOACs do not have the variation in behaviour that warfarin does and so they do not need regular blood tests to monitor their effect. There is now increasing evidence that the DOACs may be associated with a lower risk of bleeding in the brain than warfarin and they are becoming increasingly used as the treatment of first line.
We have pioneered research in the use of these drugs to protect patients during ablation and now do all of our ablations on these drugs without interrupting them. We have found that the risk of bleeding complication is actually less when using these drugs than when interrupting them and replacing them with short acting injections. The additional benefit is that patients spend no time without the protection of an anticoagulant and this may explain why our stroke rates are some of the lowest in the world.
If you have persistent AF (AF that does not stop on its own without treatment like a cardioversion) we may also recommend a short course of amiodarone to start a week or so before the procedure and to continue for 3 months after. Amiodarone is a very effective anti-rhythm drug which is not used routinely for long periods of time because of its potential to cause long-term cumulative side effects like thyroid problems, liver and lung fibrosis. These are not common in short term treatment.
On the Day of the Procedure
On the day of the procedure we will admit you to hospital and ensure you are ready for the procedure. If you are having the procedure under a general anaesthetic one of our anaesthetists will see you on the ward before your procedure starts.
You will be taken to the operating room known as the cardiac catheter lab and the last of 3 or 4 safety briefs and checks will take place with you and the rest of the team to ensure that everyone is happy with what the plan is and everyone knows their role in it. It is also an opportunity to check yet again that you have no allergies and are prepared for the procedure.
We will then sedate or anaesthetise you and put a local anaesthetic at the top of the leg so that when you wake up your leg is not sore.
During the Procedure
Once you are asleep we will pass an ultrasound probe down your throat to do a detailed ultrasound of the heart (known as a transoesophageal echo (TOE)). This allows us to check the heart for clot and in some patients totally eliminate the use of x-rays for your procedure.
At present for paroxysmal AF (AF that stops without needing an electric shock or cardioversion), we use a cryo (fr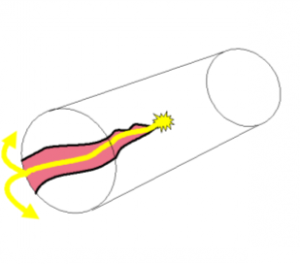 eezing) ablation balloon to isolate the electrical signals of the pulmonary veins. These veins drain blood from the lungs into the heart and electrical signals within them fire off, enter into the heart and appear to be the the source of AF in the majority of patients.
eezing) ablation balloon to isolate the electrical signals of the pulmonary veins. These veins drain blood from the lungs into the heart and electrical signals within them fire off, enter into the heart and appear to be the the source of AF in the majority of patients.
By electrically disconnecting these veins from the heart (while leaving the “plumbing” unaffected) we can eliminate AF in the majority of patients. We use the cryo balloon because we were the first in the world to show in research studies – https://www.ncbi.nlm.nih.gov/pubmed/26727045 that this is superior to radiofrequency burning in eliminating AF in patients with paroxysmal AF.
This video shows a cryoablation balloon in the right lower pulmonary vein. X-ray dye is being injected that is spilling out (so the vein is not completely occluded by the balloon yet). The dots to the left of the balloon are electrodes on a fine mapping wire passed through the balloon and into the vein. These allow us to record electrical signals during the freeze. These signals will disappear when the vein has been electrically disconnected (isolated) from the left atrium.
After the Procedure
After the procedure an echocardiogram is performed to make sure that fluid has not leaked out of the heart. A stitch is used at the top of the leg and the tubes removed. The patient is then returned to their room for close monitoring by the nursing staff. They will ask you to lie flat for a period of time to allow the leg to heal properly. Once a clot has formed over the vein at the top of the leg, to seal it off, the stich is loosened and removed and you will be gradually mobilised. If you have bleeding problems after some patients need longer in bed to heal than others and rarely we will put a small stich back into the leg before you go home.
Risks & Possible Side Effects Post Operation
Risks are low. Minor complications (defined as something that does not need treatment and does not delay discharge home) including bruising, chest pain, recurrent AF (for a few weeks which then will often settle down), temporary damage to the nerve that supplies the diaphragm or stomach (lasting a few weeks or months before it resolves).
It is not unusual to have symptoms of chest pain and palpitation after the procedure. Even if atrial rhythm problems occur these, can often resolve on their own after 3 months. We are not sure why this happens but it seems likely that inflammation of the atrium following the ablation can be one of the reasons.
Persistent AF
For persistent AF, sometimes a more extensive ablation may be necessary so if you are not one of the 50% of patients with persistent AF where cryoballoon ablation alone has not worked and the AF comes back we use RF energy to repeat the procedure and allow us to perform a more extensive procedure. For RF ablation we use a 3D mapping system which allows us to create a computer model of the heart (hyperlink to video here) and place the lesions with great accuracy and avoid the use of X-rays. Indeed, professor Schilling has pioneered X-ray free AF ablation.
This video shows the creation of the left atrial geometry. This is done by dragging the catheter around the left atrium and a geometry of the left atrium is created where the catheter has been. Once the catheter has been dragged across the whole chamber it has created a complete model of the geometry. The system knows where the catheter is using a 3D navigation (similar to a very precise GPS system). Because the catheter is soft, can be seen on the 3D mapping system and because I know where the veins and other anatomy are relative to one another, this can be done without any x-ray.
Professor Schilling’s group was one of the first in the world to demonstrate that performing ablation on anticoagulant drugs is actually safer than interrupting them. For this reason we will ask to remain on your stroke prevention medication throughout the time of the procedure and for at least 3 months after.
Assuring the Best Results
Professor Schilling regularly has his own results audited and publishes them. This allows him to make subtle changes to his technique to refine and improve these outcomes.
As you can see from his results, some patients need more than one procedure to get the best results.
